Genital Prolapse at DRHC Dubai
What is Female Genital Prolapse?
Female genital prolapse (or pelvic organ prolapse) is characterized by a portion of the vaginal canal protruding (prolapsing) from the opening of the vagina. The condition usually occurs when the pelvic floor collapses as a result of multiple childbirths, which can tear soft tissues or hysterectomy, so that the vaginal wall collapses, resulting in cystocele, rectocele, or both. This is a common gynecological condition, but many women do not seek treatment because of embarrassment.
It is important to underline that it is a completely treatable problem, so seeking medical advice at an early stage is strongly advised to solve the problem without a surgical operation being necessary.
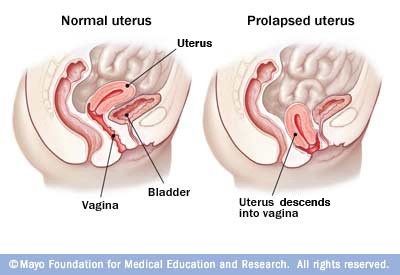
Female Genital Prolapse Classification
Grading
Prolapse of the uterus can occur on its own, but it can also be associated with a vaginal protrusion. The degree of prolapse can vary from a very mild descent of the pelvic organs to a severe descent in which the uterus, part of the bladder, and part of the rectum protrude through the vaginal opening.
Pelvic organ prolapses are graded either via the Baden-Walker System, Shaw's System, or the Pelvic Organ Prolapse Quantification (POP-Q) System.
We normally use the POP-Q system as follows:
| Stage |
description |
| 0 |
No prolapse anterior and posterior points are all 3cm, and C or D is between -TVL and -(TVL-2) cm. |
| 1 |
The criteria for stage 0 are not met, and the most distal prolapse is more than 1cm above the level of the hymen (less than -1 cm). |
| 2 |
The most distal prolapse is between 1cm above and 1cm below the hymen (at least one point is -1, 0, or +1). |
| 3 |
The most distal prolapse is more than 1cm below the hymen but no further than 2cm less than TVL. |
| 4 |
Represents complete procidentia or vault eversion; the most distal prolapse protrudes to at least (TVL-2) cm. |
What Causes the Prolapse?
This is due to a weakness in the supporting tissues of the pelvic floor.
The common leading factors are:
- Pregnancy and Childbirth: for excessive stretching of the tissues and tears of the soft tissues and muscles
- Surgical asportation of the uterus: During the operation, most of the uterine supporting structures are also removed
- After menopause: a relative lack of female hormones can lead to the thinning and weakening of the tissues
- Any condition that leads to an increase in pressure in the abdominal cavity (e.g., chronic cough, constipation, or heavy lifting) can aggravate the prolapse.
What Are The Symptoms Of Utero-Vaginal Prolapse?
Some women with a very mild degree of prolapse may not have any symptoms at all. However, most women with significant prolapse may experience some of the following:
- Discomfort in the lower abdomen or pelvis
- The sensation of swelling or fullness in the vagina
- Difficulty in passing motion or urine
- Urinary incontinence
- Fecal incontinence
- Frequent bladder infections
- Pain during intercourse
Many of the above symptoms are relieved when lying down and are worse in the evening and better in the morning.
How Can It Be Prevented?
Prevention has a key role in female genital prolapse since strengthening pelvic muscles with biofeedback helps to avoid pelvic floor descent.
So we strongly recommend during pregnancy and after childbirth to do pelvic floor exercises, to avoid any problems and to help new mothers easily get back to their normal pelvic anatomy.
In our center, we offer pelvic floor exercise courses and a free babysitting service for new mothers
We also offer customized courses for women in menopause to prevent and treat urinary and fecal incontinence.
Female Genital Prolapse Treatment
Non-Surgical Treatment
The milestone of female genital prolapse medical therapy is biofeedback and pelvic floor rehabilitation.
In the most advanced cases, when the patient is not willing to undergo surgery, there are many different types of vaginal pessaries available that can be inserted into the vagina to support the prolapse and temporarily relieve the symptoms.
In the menopause, estrogen-containing cream to apply to the vagina is also very helpful.
Surgical Treatment
Surgery is curative for female genital prolapse. The principles of surgery are to correct the supportive defects and restore normal anatomy and sexual function. This may include hitching up the bladder and/or uterus and/or vagina, or repair and 'tightening' of the vagina. Depending on the condition, surgery may be performed either through the vagina or through the abdomen.
.png?width=281&height=59&name=bookanappointment%20(1).png)
In DRHC Dubai, we are proud to offer the latest minimally invasive techniques to guarantee our patients a painless postoperative course and a very short recovery time. To book your appointment, please call +97142798200 today!




.png?width=281&height=59&name=bookanappointment%20(1).png)




