Thyroidectomy at DRHC Dubai Thyroid Clinic
At Dr. Rami Hamed Center in DRHC, we provide the leading thyroid specialist in Dubai for complete care of thyroid diseases, including all diagnostic modalities and the latest non-surgical and surgical techniques available for the best outcomes
How to Perform a ‘Safe’ Thyroidectomy
Reviewing the steps needed to perform a'safe' thyroidectomy as well as providing several hints that can assure safe passage through the anatomical difficulties during thyroid surgery.
Additional preoperative issues specific to thyroid surgery
Based on the patient’s medical history, consultations for cardiac, respiratory, metabolic, and other specialties may be necessary. Thyroid imaging studies (ultrasound, CT, MRI), thyroid function tests, and perioperative antibiotics are usually not indicated except in some special circumstances. The preoperative surgery performed is a useful adjunctive measure, as it helps the surgeon visualize the thyroid gland and its pathology and provides guidance for the incision. If the patient complains of voice problems, a preoperative laryngoscopy will be needed to document vocal fold mobility.
Intraoperative Considerations for Thyroidectomy:
1 - Patient positioning: The patient is placed in the supine position on the operating room table with a slight extension of the neck (11–15°). It is important to verify that the neck is not hyperextended because patients may experience severe neck and upper back pain following surgery.
2 - Incision placement: A transverse cervical incision is used most commonly for either thyroid lobectomy or total thyroidectomy. The incision is made in the direction of Langer’s lines in order to minimize scarring and improve the cosmetic appearance of the scar.
3: Raising skin flaps and mobilizing strap muscles: Exposing the cranial portion of the strap muscles allows for easier identification of the midline, especially in the case of young patients whose midline is less well-defined due to well-developed strap muscles.
4 - Dividing the isthmus
5 - Division of the superior pole vessels: Careful dissection and separate ligation of the branches of the artery and vein ensure effective hemostasis and avoid inadvertent retraction of small vessels that could cause life-threatening bleeding postoperatively.
6 - Identification of the recurrent laryngeal nerve and parathyroid glands and mobilization of the lower pole vessels: If a nerve stimulator device is used, try to map out the RLN based on its anatomical relationship to the parathyroid glands. This allows for minimal dissection around the nerve and helps prevent nerve traction injury to help retract a large goiter extending inferiorly below the clavicle 0-chromic sutures can be placed in the thyroid parenchyma and the thyroid is retracted cranially and medially.
7 - Berry’s ligament, haemostasis: The final step before removing the thyroid is to separate the gland from the anterior surface of the trachea by dividing Berry’s ligament. This can be done either by LigaSure, electrosurgical instruments, or sharply with Metzenbaum scissors or a scalpel.
8 - Closure: You may ask the anaesthesiologist to initiate a Valsalva maneuver up to a pressure of 30–35 mmHg. However, this does not eliminate the risk of postoperative bleeding. It may find small vessels that might have been improperly sealed or litigated.
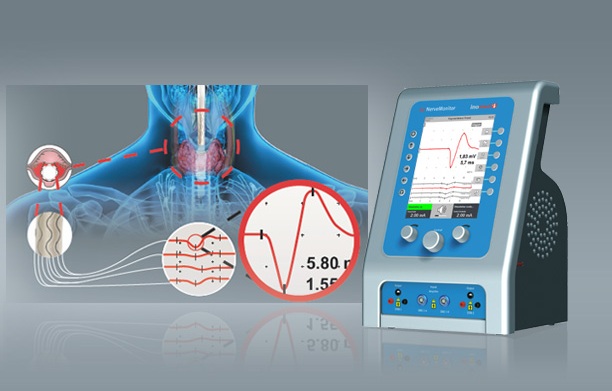
Neuromonitoring in Thyroid Surgery:
Injuries of the vocal nerves (recurrent laryngeal nerves) are one of the severe complications of thyroid surgery. Unilateral injury causes hoarseness and to some extent, even breathing disorders.
On the other hand, bilateral nerve injuries cause asphyxia. Protection of the recurrent laryngeal nerves (vocal nerves) is a major concern of the surgeon. A combination of experience and neuromonitoring definitely reduces the incidence of injury.
That is why, a neuromonitoring system was developed for such purposes to minimize the risk of injury of the vocal cords. It showed advantages in many selected cases, for example, reoperations or total thyroidectomy.
Stimulation of the vagus nerve provides a more accurate analysis of the recurrent laryngeal nerve than that of a distal segment of the recurrent laryngeal nerve alone. The main purpose is a permanent neuromonitoring of the vagus nerve through continuous electrical stimulations.
Intraoperative neuromonitoring gives us a rapid identification and location of the recurrent laryngeal nerve and even its variations. This allows the protection of functional integrity and lowers the incidence of injury.
Principles of intraoperative neuromonitoring:
The motor nerves are stimulated by electricity during the procedure. The nerve impulses which are formed will be transformed to the muscles so that myoelectric signals are produced forming waves in the electromyography.
.png?width=281&height=59&name=bookanappointment%20(1).png)
Dubai Thyroid Clinic - DRHC provides treatment for hypothyroidism, hyperthyroidism, thyroid cancer, thyroid disease, thyroidectomy, and thyroid surgery. To book your Appointment please call +97142798200.



.png?width=281&height=59&name=bookanappointment%20(1).png)
.webp?width=1080&height=1080&name=Doctor%20background%20For%20Website%20Dr.%20Fadi%20Nageeb%2009%20(1).webp)
.webp?width=1080&height=1080&name=Doctor%20background%20For%20Website%20Dr%20Abdul%20Majeed%20Khalid%20%2002%20(1).webp)



